Colles fracture definition12/25/2023  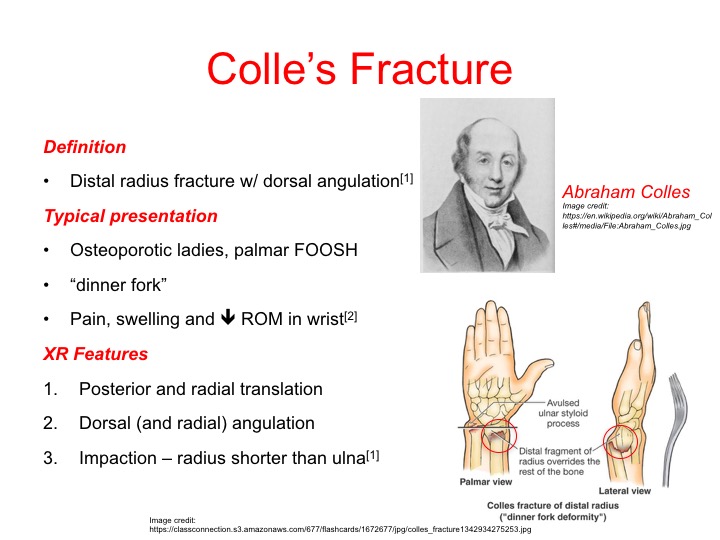 
Alternative methods of fracture reduction involve simulating the injurious impact by worsening the deformity, disengaging fracture ends, and angulation correction using the distraction force. By applying traction, intact tendons, muscles, and periosteum may immediately reduce regions of fracture comminution. Alternative fracture manipulation techniques are needed for displaced fractures with periosteal hinges and fractures that do not align with traction. Translation of the bone ends during distraction allows fracture reduction. The amount of traction applied should be greater than the magnitude of the muscle spasm. The closed reduction of a displaced fracture requires initial distraction, deformity alignment by connecting the bone ends, and length stabilization. Sustained gentle traction that can stretch the soft tissue surrounding the fracture to realign the bony ends is required. Pain that persists after rest, splinting, elevation, and adequate analgesia may indicate compartment syndrome, which requires surgical consultation. Parenteral analgesics should be administered before and after fracture manipulation and splint application to relieve pain without significant sedation. However, most patients do not seek care until hours after the fracture, when the hematoma has already formed and cannot be aspirated. Hematoma blocks are not appropriate for patients with open fractures. The hematoma will function as a fluid medium, allowing the anesthetic to diffuse within the fracture site. Inject 5 to 10 mL of local anesthesia into the fracture. Aspirate as much of the hematoma as possible. Aspiration of blood and fat droplets confirms the correct position of the needle. To perform a hematoma block, insert a needle into the fracture site after palpating the fracture ends. A viable substitute for regional anesthesia is the hematoma block. Children are more likely to require general anesthesia than adults, most of whom will tolerate the procedure with regional anesthesia and adjunctive analgesia. Using analgesics and anesthesia ensures comfort and muscle relaxation to reduce a fracture and apply a splint effectively. The manipulation of acute fractures is painful. Although plaster is considered the traditional splinting material, padded fiberglass or preformed plastic splints are commonly encountered in clinical practice. Splinting may be the definitive treatment or temporary treatment before casting. Splints can be easily removed for wound care. Splints differ from casts in that the noncircumferential bandage allows for some degree of soft tissue swelling without undue constriction. Splints may be used for comfort as a temporizing measure for wrist and hand dislocations or fracture subluxations while awaiting definitive care. 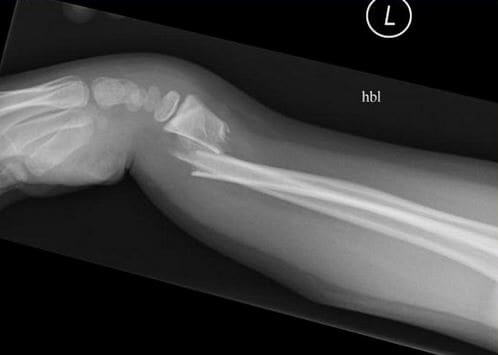
Splinting improves patient comfort, facilitates recovery, and protects from further injury. Splinting is an adjunct to elevation and ice. Other conditions amenable to volar splinting include acute gouty arthritis, carpal tunnel syndrome, and radial nerve palsy. For more proximal shaft fractures, the principle of volar splinting expands into sugar-tong or Muenster-type splinting, extending above the elbow. Exceptions to this rule include metaphyseal fractures, such as Colles or Smith fractures metaphyseal fractures behave like injuries within the joint. Basic splinting guidelines of skeletal pathology require immobilization of the joint above and below the lesion. Hard tissue skeletal injuries that may benefit from volar splinting include distal radius fractures, Colles fractures, and metacarpal or carpal fractures, excluding fractures of the first metacarpal and trapezium. Volar splinting of the upper extremity can be employed to immobilize hard and soft tissue injuries in addition to painful atraumatic conditions. This activity reviews the indications, contraindications, complications, and technique of volar splinting and highlights the role of the interprofessional team in caring for patients with upper extremity injuries that may benefit from volar splinting. However, volar splinting for chronic conditions may assist the healing process, provide long-term pain control, and slow the progression of the underlying pathophysiological process. Volar splinting is generally limited to short-term use to maximize benefits while minimizing complications. Volar splinting can immobilize and protect the affected upper extremity, facilitate healing, and decrease pain. Splints allow for soft tissue swelling in the acute phase of healing. In general, splinting is useful for various conditions, including fractures, sprains, strains, reduced fracture-dislocations, and after extensive laceration repair. Volar splinting of the upper extremity can be employed to immobilize hard and soft tissue injuries and painful atraumatic conditions. 
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
